Launched at this time, the newest section of the Covid-19 inquiry report investigated the affect of the pandemic on UK well being methods.
Its findings recommend the NHS was not solely examined but in addition ill-prepared, plunging it right into a precarious state amid the calls for of the pandemic.
Within the years main as much as the pandemic, NHS budgets had been tightly squeezed, leaving methods struggling to deal with a surge of patients desperately in search of assist.
Listed below are the important thing takeaways of at this time’s report.
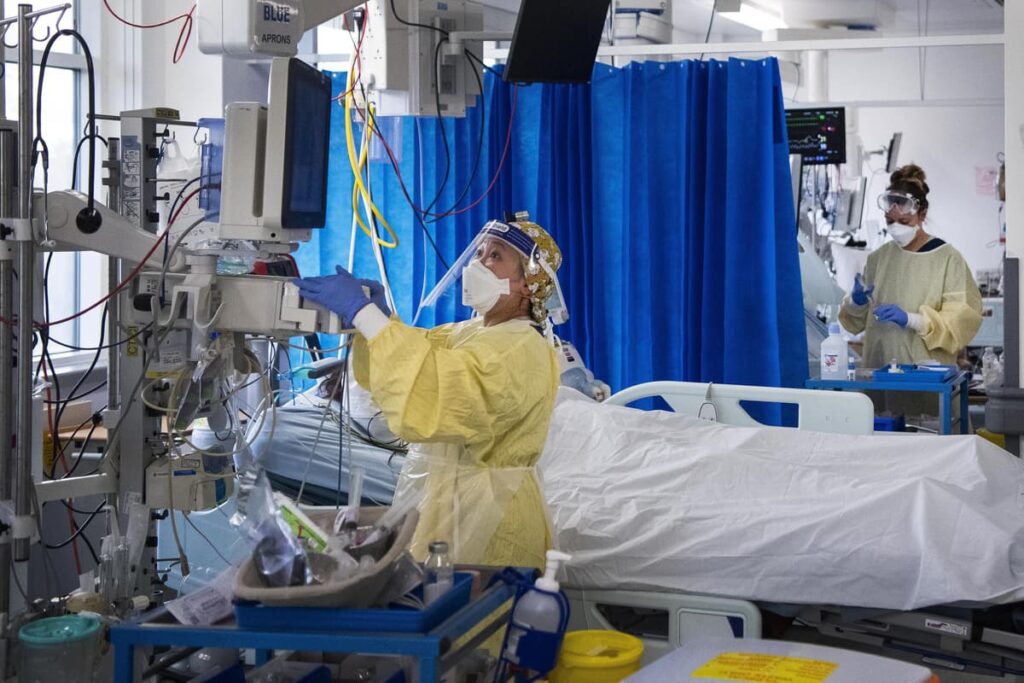
Nurses caring for Covid-19 sufferers within the Intensive Care Unit (ICU) in St George’s Hospital in Tooting, south-west London in July 2021
PA
1. The NHS got here near collapse
In response to the inquiry, “healthcare methods had been overwhelmed and got here near collapse” as well being care services virtually buckled beneath the pandemic pressure.
The NHS solely obtained by the pandemic due to the “extraordinary efforts of all these working in healthcare throughout the UK”.
Baroness Hallett DBE, who shared a gap assertion for the inquiry, described the UK response as “we coped, however solely simply”.
2. Paused most cancers screenings led to deaths
With hospitals overwhelmed, different healthcare providers suffered throughout the pandemic.
Amongst them had been most cancers screening providers, which had been paused in components of the UK, resulting in a “steep drop in analysis in 2020”.
The report says: “Missed and late diagnoses and longer waits for remedy for colorectal most cancers throughout the pandemic resulted in lack of life and elevated mortality charges.”
The backlog for screenings and most cancers diagnoses various considerably throughout the UK, including to “prolonged ready lists”.
3. Politicians had been ‘reluctant to just accept’ the NHS was ‘overwhelmed’
In a gap assertion by Baroness Hallett, one statement was the reluctance amongst politicians to just accept the fact unfolding in UK healthcare settings.
She additionally named Matt Hancock, the Well being Secretary on the time.
“Politicians, together with the Secretary of State for Well being and Social Care, Matt Hancock, had been reluctant to just accept that healthcare methods had been ‘overwhelmed’, as they selected this to imply whole collapse,” she mentioned.
Baroness Hallett continued: “In my opinion, it’s a query of semantics. No matter phrase one chooses, healthcare methods had been positioned beneath insupportable pressure.”
4. London reported ‘CRITCON 4’ 4 instances in early pandemic
Hospitals had been required to report their CRITCON stage throughout the pandemic to watch the pressure beneath which hospitals are positioned.
CRITCON 4 is the very best stage, “emergency”, which describes conditions larger than “unprecedented” and “full stretch”.
In response to the report: “CRITCON 4 means primarily the entire [intensive care] system can’t offload …
nowhere is full till in all places is full – nowhere is overwhelmed, slightly, till in all places is overwhelmed.”
Nevertheless, it’s unclear whether or not there could have been discrepancies in preliminary reporting, with some folks stating overwhelmed services could not have reported CRITCON 4, whereas others did so by mistake.
The report says: “The Inquiry was instructed that NHS England believed a number of of the CRITCON 4 declarations in Determine 17 had been made in error.”
5. Ladies and ethnic minorities within the NHS much less prone to have entry to becoming masks
Ladies and ethnic minority employees had been much less protected towards contracting Covid-19, in keeping with the report. That is reportedly as a result of that they had “much less alternative” to get acceptable FFP3 masks whereas working in comparison with their “white, male colleagues”.
In response to the report, “given the massive share of feminine and ethnic minority healthcare staff working in
the NHS and the dearth of entry to FFP3 masks that had been designed to suit their facial shapes, girls and ethnic minority healthcare staff had been extra prone to be left inadequately protected.”
About 45 per cent of the NHS workforce in London comes from ethnic minority backgrounds.
Extra broadly, there have been additionally larger mortality charges amongst ethnic minority teams, with Sir Christopher Whitty including this was “largely to do with the place the waves had been at their worst. So within the first wave, London, which has a big proportion of the British black inhabitants, and the second wave, the Midlands, the place a better proportion of the British Asian inhabitants dwell.”
6. London hospital capacities prompted the launch of Nightingale hospitals
Shortly earlier than the primary lockdown, there was already concern that London could be the primary UK metropolis to exceed hospital capability.
London had 800 intensive care beds on the time, however modelling projected round 4,000 could be wanted.
“Whereas it was anticipated that the opposite surge measures examined on this chapter would assist to extend intensive care capability, it was apparent that this capability wanted to be elevated but additional,” the report reads, prompting early discussions concerning the institution of the Nightingale hospitals.
7. Keep at house recommendation deterred folks from in search of medical consideration
The report additionally claims folks had been “deterred from accessing healthcare”, partly attributable to public messaging.
Though the “keep at house” recommendation shared with the general public throughout the pandemic was “meant to maintain them secure,” the report says lots of people “didn’t need to ‘overburden’ the NHS”.
This will point out that messaging was complicated to some and “inadvertently despatched the message that healthcare was closed”.
8. London nursing ratios stretched throughout pandemic
Highlighting not solely the unbelievable resilience of nursing employees but in addition the sheer stress beneath which they had been positioned, the inquiry exhibits that nursing ratios had been stretched dramatically throughout the pandemic.
A variety of London hospitals needed to stretch their nursing ratios throughout the pandemic, with the Queen Elizabeth Hospital working with one nurse to each 4 sufferers.
In the meantime, within the Royal London Hospital (Barts Well being NHS Belief), the radio stretched to at least one nurse for each 5 sufferers, whereas some intensive care items “reached one specialist care nurse to 6 mechanically ventilated sufferers”.
9. ‘Horrible trade-offs had been required’
The report additionally highlights that, given the quantity of Covid-19 circumstances, “horrible trade-offs had been required,” comparable to stopping folks from visiting family members on the finish of their lives.
This has had a “devastating affect on bereaved relations”.
The report added: “This was a specific concern within the early phases of the pandemic, the place restrictions meant that many sufferers died with out the consolation of being surrounded by their family members and had been disadvantaged of the chance
to say goodbye.”